
Introduction
Coma is a medical condition characterized by a prolonged state of unconsciousness. It is a serious and life-threatening condition that requires immediate medical attention.[1][2] The aim of this guide is to provide healthcare professionals with a comprehensive overview of the diagnostic steps and possible interventions for coma.
Codes
Symptoms
- Altered level of consciousness: The patient is unresponsive and does not react to external stimuli.[5]
- Absence of purposeful movements: The patient does not exhibit voluntary movements.[6]
- Abnormal eye movements: The patient may have fixed or roving eye movements.[7]
- Abnormal breathing patterns: The patient may exhibit irregular or abnormal breathing patterns.[8]
Causes
- Traumatic brain injury: A severe blow to the head can cause brain damage and result in coma.[9]
- Stroke: A disruption of blood flow to the brain can lead to coma.[10]
- Infections: Certain infections, such as meningitis or encephalitis, can cause inflammation of the brain and result in coma.
- Drug overdose: Overdosing on certain medications or illicit drugs can lead to coma.
- Metabolic disorders: Conditions such as diabetic ketoacidosis or liver failure can cause coma.
Diagnostic Steps
Medical History
- Gather information about the patient’s risk factors, such as a history of head trauma, drug use, or underlying medical conditions.
- Inquire about the onset and duration of the coma.
- Ask about any preceding symptoms or events that may have triggered the coma.
Physical Examination
- Assess the patient’s vital signs, including heart rate, blood pressure, and respiratory rate.
- Perform a neurological examination to evaluate the patient’s level of consciousness, pupillary response, and motor responses.
- Check for any signs of trauma or injury, such as bruising or swelling.
Laboratory Tests
- Complete blood count (CBC): To assess for any signs of infection or anemia.
- Blood glucose level: To rule out hypoglycemia or hyperglycemia as a cause of coma.
- Electrolyte levels: To evaluate for any imbalances that may contribute to the coma.
- Liver function tests: To assess liver function and rule out hepatic encephalopathy.
- Toxicology screen: To detect the presence of drugs or toxins in the patient’s system.
Diagnostic Imaging
- Computed tomography (CT) scan: To evaluate for any structural abnormalities or bleeding in the brain.
- Magnetic resonance imaging (MRI): To obtain more detailed images of the brain and assess for any underlying pathology.
- Electroencephalogram (EEG): To evaluate brain activity and detect any abnormal electrical patterns.
Other Tests
- Lumbar puncture: To obtain cerebrospinal fluid for analysis and rule out infections.
- Evoked potentials: To assess the function of specific sensory pathways in the brain.
- Biopsy: In certain cases, a brain biopsy may be necessary to determine the underlying cause of the coma.
Follow-up and Patient Education
- Provide appropriate supportive care to the patient, including monitoring vital signs and ensuring a stable environment.
- Educate the patient’s family members about the condition, prognosis, and potential treatment options.
- Arrange for appropriate rehabilitation services if the patient recovers from the coma.
Possible Interventions
Traditional Interventions
Medications:
Top 5 drugs for coma:
- Mannitol:
- Cost: $10-$50 per vial.
- Contraindications: Severe dehydration, renal failure.
- Side effects: Fluid and electrolyte imbalances, kidney damage.
- Severe side effects: Pulmonary edema, heart failure.
- Drug interactions: None reported.
- Warning: Close monitoring of fluid and electrolyte balance is required.
- Phenytoin:
- Cost: $10-$50 per vial.
- Contraindications: Hypersensitivity to phenytoin, heart block.
- Side effects: Nausea, dizziness, rash.
- Severe side effects: Stevens-Johnson syndrome, toxic epidermal necrolysis.
- Drug interactions: Many drug interactions, including anticoagulants and antiepileptic drugs.
- Warning: Regular monitoring of blood levels is required.
- Propofol:
- Cost: $20-$100 per vial.
- Contraindications: Hypersensitivity to propofol, egg or soy allergy.
- Side effects: Hypotension, respiratory depression.
- Severe side effects: Propofol infusion syndrome, anaphylaxis.
- Drug interactions: None reported.
- Warning: Should be administered by trained healthcare professionals in a monitored setting.
- Midazolam:
- Cost: $10-$50 per vial.
- Contraindications: Hypersensitivity to midazolam, acute narrow-angle glaucoma.
- Side effects: Sedation, respiratory depression.
- Severe side effects: Paradoxical reactions, cardiac arrest.
- Drug interactions: Many drug interactions, including opioids and other sedatives.
- Warning: Should be administered with caution in patients with respiratory or liver impairment.
- Naloxone:
- Cost: $20-$100 per vial.
- Contraindications: Hypersensitivity to naloxone, opioid dependence.
- Side effects: Nausea, vomiting, increased blood pressure.
- Severe side effects: Seizures, pulmonary edema.
- Drug interactions: None reported.
- Warning: Close monitoring of the patient’s response is required.
Alternative Drugs:
- Barbiturates (e.g., Phenobarbital): Used in certain cases to induce therapeutic coma.
- Diazepam: May be used as an alternative to midazolam for sedation.
- Lorazepam: Another alternative to midazolam for sedation.
- Haloperidol: Used to manage agitation or delirium in coma patients.
- Levetiracetam: An antiepileptic drug that may be used in cases of coma due to seizures.
Surgical Procedures:
- Craniotomy: In cases of traumatic brain injury or intracranial hemorrhage, a craniotomy may be performed to relieve pressure on the brain.
- Ventriculostomy: In cases of hydrocephalus or increased intracranial pressure, a ventriculostomy may be performed to drain excess cerebrospinal fluid.
- Decompressive hemicraniectomy: In cases of severe brain swelling, a portion of the skull may be removed to relieve pressure on the brain.
Alternative Interventions
- Hyperbaric oxygen therapy: Involves breathing pure oxygen in a pressurized chamber to increase oxygen delivery to the brain. Cost: $200-$300 per session.
- Transcranial magnetic stimulation (TMS): Non-invasive procedure that uses magnetic fields to stimulate nerve cells in the brain. Cost: $300-$500 per session.
- Acupuncture: May help improve blood flow and promote healing. Cost: $60-$120 per session.
- Music therapy: Listening to music may have a calming effect and promote relaxation. Cost: Varies depending on the provider.
- Hypnotherapy: May help reduce stress and promote a sense of well-being. Cost: $75-$150 per session.
Lifestyle Interventions
- Provide a quiet and calm environment for the patient.
- Ensure proper nutrition and hydration.
- Encourage physical therapy and rehabilitation exercises.
- Promote good sleep hygiene.
- Provide emotional support to the patient and their family.
It is important to note that the cost ranges provided are approximate and may vary depending on the location and availability of the interventions.
Mirari Cold Plasma Alternative Intervention
Understanding Mirari Cold Plasma
- Safe and Non-Invasive Treatment: Mirari Cold Plasma is a safe and non-invasive treatment option for various skin conditions. It does not require incisions, minimizing the risk of scarring, bleeding, or tissue damage.
- Efficient Extraction of Foreign Bodies: Mirari Cold Plasma facilitates the removal of foreign bodies from the skin by degrading and dissociating organic matter, allowing easier access and extraction.
- Pain Reduction and Comfort: Mirari Cold Plasma has a local analgesic effect, providing pain relief during the treatment, making it more comfortable for the patient.
- Reduced Risk of Infection: Mirari Cold Plasma has antimicrobial properties, effectively killing bacteria and reducing the risk of infection.
- Accelerated Healing and Minimal Scarring: Mirari Cold Plasma stimulates wound healing and tissue regeneration, reducing healing time and minimizing the formation of scars.
Mirari Cold Plasma Prescription
Video instructions for using Mirari Cold Plasma Device – A07 Coma (ICD-10:R40.2)
| Mild | Moderate | Severe |
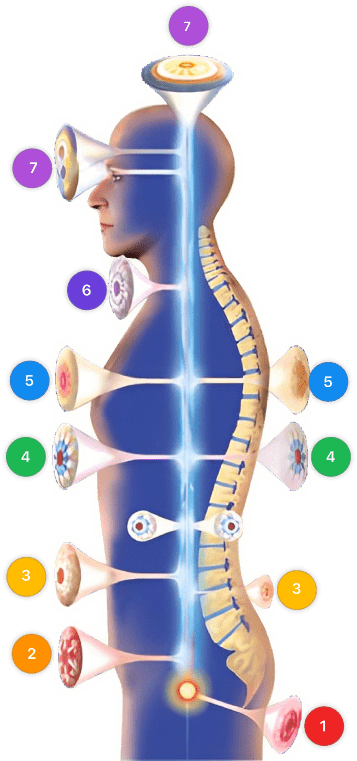
| Mode setting: 7 (Immunotherapy) Location: 1 (Sacrum) Morning: 15 minutes, Evening: 15 minutes |
Mode setting: 7 (Immunotherapy) Location: 1 (Sacrum) Morning: 30 minutes, Lunch: 30 minutes, Evening: 30 minutes |
Mode setting: 7 (Immunotherapy) Location: 1 (Sacrum) Morning: 30 minutes, Lunch: 30 minutes, Evening: 30 minutes |
| Mode setting: 7 (Immunotherapy) Location: 4 (Heart, Bile & Pancreas) Morning: 15 minutes, Evening: 15 minutes |
Mode setting: 7 (Immunotherapy) Location: 4 (Heart, Bile & Pancreas) Morning: 30 minutes, Lunch: 30 minutes, Evening: 30 minutes |
Mode setting: 7 (Immunotherapy) Location: 4 (Heart, Bile & Pancreas) Morning: 30 minutes, Lunch: 30 minutes, Evening: 30 minutes |
| Mode setting: 7 (Immunotherapy) Location: 7 (Neuro system & ENT) Morning: 15 minutes, Evening: 15 minutes |
Mode setting: 7 (Immunotherapy) Location: 7 (Neuro system & ENT) Morning: 30 minutes, Lunch: 30 minutes, Evening: 30 minutes |
Mode setting: 7 (Immunotherapy) Location: 7 (Neuro system & ENT) Morning: 30 minutes, Lunch: 30 minutes, Evening: 30 minutes |
| Total Morning: 45 minutes approx. $7.50 USD, Evening: 45 minutes approx. $7.50 USD |
Total Morning: 90 minutes approx. $15 USD, Lunch: 90 minutes approx. $15 USD, Evening: 90 minutes approx. $15 USD, |
Total Morning: 90 minutes approx. $15 USD, Lunch: 90 minutes approx. $15 USD, Evening: 90 minutes approx. $15 USD, |
| Usual treatment for 7-60 days approx. $105 USD – $900 USD | Usual treatment for 6-8 weeks approx. $1,890 USD – $2,520 USD |
Usual treatment for 3-6 months approx. $4,050 USD – $8,100 USD
|
 |
|
Use the Mirari Cold Plasma device to treat Coma effectively.
WARNING: MIRARI COLD PLASMA IS DESIGNED FOR THE HUMAN BODY WITHOUT ANY ARTIFICIAL OR THIRD PARTY PRODUCTS. USE OF OTHER PRODUCTS IN COMBINATION WITH MIRARI COLD PLASMA MAY CAUSE UNPREDICTABLE EFFECTS, HARM OR INJURY. PLEASE CONSULT A MEDICAL PROFESSIONAL BEFORE COMBINING ANY OTHER PRODUCTS WITH USE OF MIRARI.
Step 1: Cleanse the Skin
- Start by cleaning the affected area of the skin with a gentle cleanser or mild soap and water. Gently pat the area dry with a clean towel.
Step 2: Prepare the Mirari Cold Plasma device
- Ensure that the Mirari Cold Plasma device is fully charged or has fresh batteries as per the manufacturer’s instructions. Make sure the device is clean and in good working condition.
- Switch on the Mirari device using the power button or by following the specific instructions provided with the device.
- Some Mirari devices may have adjustable settings for intensity or treatment duration. Follow the manufacturer’s instructions to select the appropriate settings based on your needs and the recommended guidelines.
Step 3: Apply the Device
- Place the Mirari device in direct contact with the affected area of the skin. Gently glide or hold the device over the skin surface, ensuring even coverage of the area experiencing.
- Slowly move the Mirari device in a circular motion or follow a specific pattern as indicated in the user manual. This helps ensure thorough treatment coverage.
Step 4: Monitor and Assess:
- Keep track of your progress and evaluate the effectiveness of the Mirari device in managing your Coma. If you have any concerns or notice any adverse reactions, consult with your health care professional.
Note
This guide is for informational purposes only and should not replace the advice of a medical professional. Always consult with your healthcare provider or a qualified medical professional for personal advice, diagnosis, or treatment. Do not solely rely on the information presented here for decisions about your health. Use of this information is at your own risk. The authors of this guide, nor any associated entities or platforms, are not responsible for any potential adverse effects or outcomes based on the content.
Mirari Cold Plasma System Disclaimer
- Purpose: The Mirari Cold Plasma System is a Class 2 medical device designed for use by trained healthcare professionals. It is registered for use in Thailand and Vietnam. It is not intended for use outside of these locations.
- Informational Use: The content and information provided with the device are for educational and informational purposes only. They are not a substitute for professional medical advice or care.
- Variable Outcomes: While the device is approved for specific uses, individual outcomes can differ. We do not assert or guarantee specific medical outcomes.
- Consultation: Prior to utilizing the device or making decisions based on its content, it is essential to consult with a Certified Mirari Tele-Therapist and your medical healthcare provider regarding specific protocols.
- Liability: By using this device, users are acknowledging and accepting all potential risks. Neither the manufacturer nor the distributor will be held accountable for any adverse reactions, injuries, or damages stemming from its use.
- Geographical Availability: This device has received approval for designated purposes by the Thai and Vietnam FDA. As of now, outside of Thailand and Vietnam, the Mirari Cold Plasma System is not available for purchase or use.
References
- Coma – Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/coma/symptoms-causes/syc-20371099
- Coma – Wikipedia. https://en.wikipedia.org/wiki/Coma
- ICPC-2 Codes – RxReasoner. https://www.rxreasoner.com/icpc2codes/component/S
- ICD-10 Code for Coma, unspecified R40.2 – AAPC. https://www.aapc.com/codes/icd-10-codes/R40.2
- Coma – Symptoms and causes – Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/coma/symptoms-causes/syc-20371099
- Coma – Symptoms – NHS. https://www.nhs.uk/conditions/coma/
- Coma: Types, Causes, Treatments, Prognosis – WebMD. https://www.webmd.com/brain/coma-types-causes-treatments-prognosis
- Coma – StatPearls – NCBI Bookshelf. https://www.ncbi.nlm.nih.gov/books/NBK430722/
- Traumatic Brain Injury and Coma – Brain Injury Association of America. https://www.biausa.org/brain-injury/about-brain-injury/nidilrr-publications/traumatic-brain-injury-and-coma
- Stroke and Coma – American Stroke Association. https://www.stroke.org/en/about-stroke/effects-of-stroke/cognitive-and-emotional-effects/coma
Related articles
Made in USA





























