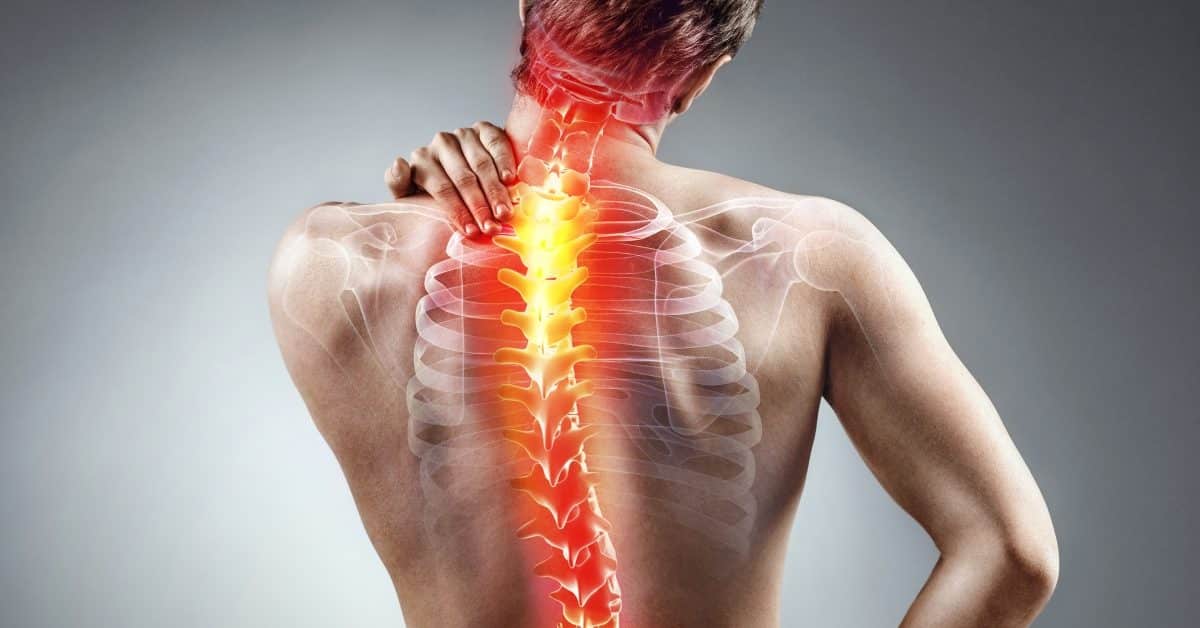
What causes acute pain affects millions worldwide seeking immediate relief from sudden, intense discomfort threatening daily life[1][2]. Acute pain causes include injury, surgery, illness, trauma, and painful medical procedures, serving as the body’s warning system of disease or threat[33]. The most common triggers are strained muscles, broken bones, dental work, infections, burns, and surgery[1][2]. The causes of acute abdominal pain encompass appendicitis, kidney stones, gallstones, and infections, while acute chest pain causes include heart attacks, lung issues, and muscle strains[12][7]. Understanding acute pain triggers helps patients recognize when immediate medical attention is needed and prevents chronic complications.
Modern medicine emphasizes identifying and treating underlying causes rather than masking symptoms.
Primary Causes of Acute Pain
Injury- and Trauma-Related Causes
Injury represents the most common acute pain cause, accounting for numerous emergency department visits[4]. These sudden-onset incidents create immediate tissue damage requiring the body’s protective response.
Common injury mechanisms include:
- Motor vehicle accidents causing multiple trauma
- Sports injuries from sudden movements or impacts
- Falls resulting in fractures or soft tissue damage
- Workplace accidents involving cuts, burns, or crushing injuries[5][11]
Specific injury types causing acute pain:
- Fractures and broken bones from high-impact trauma
- Sprains and strains affecting ligaments and muscles
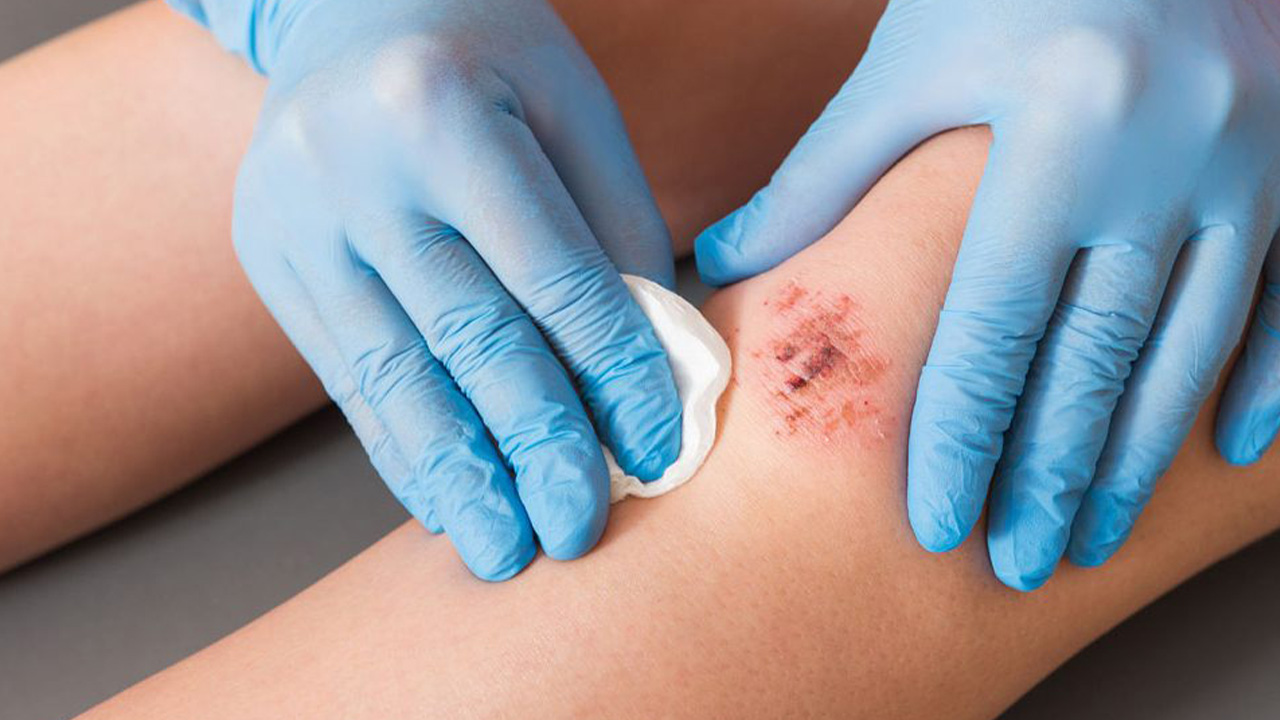
- Cuts and lacerations breaking skin integrity
- Burns from heat, chemicals, or electrical sources
- Bruises and contusions from blunt force impacts[1][31]
Surgical Procedures and Medical Interventions
Surgery consistently produces acute pain as a predictable consequence of tissue manipulation and healing[2][15]. Post-surgical pain serves both protective and problematic functions.
Surgical pain characteristics:
- Immediate onset following procedures
- Localized around incision sites
- Intensity varies by procedure type and extent
- Duration correlates with tissue healing process[15]
Medical procedures causing acute pain:
- Major surgical operations requiring tissue cutting
- Dental extractions and oral surgery
- Biopsies involving tissue sampling
- Injections and intravenous procedures[30]
Disease-Related Acute Pain Causes
Infectious Conditions
Infections trigger acute pain as the body’s immune system responds to pathogens[4]. This inflammatory response creates localized discomfort, alerting patients to seek treatment.
Common infectious causes:
- Urinary tract infections causing burning and urgency
- Strep throat creating severe swallowing pain
- Pneumonia generating chest pain with breathing
- Ear infections producing intense throbbing
- Skin infections causing localized tenderness[5]
Infection-related pain mechanisms:
- Inflammatory mediators sensitizing pain receptors
- Tissue swelling creating pressure and discomfort
- Fever responses generating widespread aching
- Immune cell activity releasing pain-producing substances[15]
Acute Medical Conditions
Sudden medical conditions create emergency scenarios requiring immediate intervention[4]. These conditions often threaten organ function or life itself.
Life-threatening causes:
- Heart attacks from blocked coronary arteries
- Pulmonary embolism blocking lung circulation
- Stroke affecting brain blood supply
- Kidney stones obstructing urinary flow[12]
| Cause Category | Common Examples | Onset Pattern | Duration |
|---|---|---|---|
| Injury/Trauma | Fractures, sprains, burns[31] | Immediate | Days to months |
| Surgical | Post-operative pain[2] | Immediate after procedure | Days to weeks |
| Infectious | UTI, strep throat, pneumonia[5] | Hours to days | Until infection clears |
| Medical Emergency | Heart attack, kidney stones[12] | Sudden, severe | Variable |
Specific Causes of Acute Abdominal Pain
Emergency Abdominal Conditions
What are the causes of acute abdominal pain? It encompasses over 20 conditions, accounting for 70% of emergency presentations[12]. The most common causes are gastroenteritis (10.8%) and nonspecific abdominal pain (10.4%)[12].
Life-threatening abdominal causes:
- Ruptured abdominal aortic aneurysm—catastrophic bleeding
- Mesenteric ischemia—blocked blood flow to intestines
- Ruptured ectopic pregnancy—internal hemorrhage[18]
Common urgent causes:
- Appendicitis (3.8%)—inflamed appendix requiring surgery
- Kidney stones (4.3%)—excruciating flank pain
- Gallbladder stones (4.5%) – right upper quadrant pain
- Diverticulitis (3.8%)—inflamed bowel pockets[12]
Location-Specific Abdominal Causes
Pain location helps identify specific organ involvement and guides diagnosis[12]:
Right Upper Quadrant:
- Cholangitis, cholecystitis, cholelithiasis—biliary system
- Pneumonia—lung involvement
- Nephrolithiasis—kidney stones[12]
Left Lower Quadrant:
- Diverticulitis—colon inflammation
- Ectopic pregnancy—gynecologic emergency
- Ovarian cyst rupture—acute pelvic pain[12]
Specific Causes of Acute Chest Pain
Cardiac-Related Causes
The causes of acute chest pain include life-threatening cardiac conditions requiring immediate recognition[7][13]. Heart-related causes create characteristic pain patterns.
Serious cardiac causes:
- Heart attack—blocked coronary artery causing muscle death
- Angina—reduced blood flow creating squeezing pain
- Aortic dissection—tearing of major artery wall
- Pericarditis—inflamed heart sac causing sharp pain[7]
Pulmonary and Other Causes
Lung-related conditions frequently cause acute chest pain[7][23]:
Respiratory causes:
- Pulmonary embolism—blood clot blocking lung vessels
- Pneumonia—lung infection causing breathing pain
- Collapsed lung—air leakage creating sudden pain
- Pleurisy—inflamed lung lining[7]
Other significant causes:
- GERD—stomach acid causing burning
- Muscle strain—overuse or injury to chest muscles
- Panic attacks – anxiety causing chest tightness
- Costochondritis—inflamed rib cartilage[7]
Why Does Acute Pain Become Chronic?
Pathophysiological Transition Process
Why does acute pain become chronic? It involves discrete pathophysiological steps occurring when initial pain persists[8]. This transition process creates permanent changes in pain processing.
Key mechanisms include:
- Peripheral sensitization—heightened nerve sensitivity
- Central sensitization—spinal cord processing changes
- Microglial activation—immune cells altering brain function
- Neuroplasticity changes—permanent brain rewiring[8]
Risk factors for chronicity:
- Inadequate initial treatment allowing sensitization
- Prolonged inflammation maintaining pain signals
- Psychological factors, including anxiety and depression
- Genetic predisposition to chronic conditions[14]
Critical Time Windows
The transition typically occurs when pain persists beyond expected healing times[14]. Early intervention during acute phases prevents chronic development.
Preventive strategies:
- Aggressive acute pain management using multimodal approaches
- Early mobilization preventing disuse complications
- Psychological support addressing fear and anxiety
- Patient education about expected recovery patterns[25]
Why Is Acute Pain Protective?
Essential Warning System
Why is acute pain said to be protective in nature? Acute pain serves as the body’s essential warning system, preventing further tissue damage[15][21]. This biological alarm motivates protective behaviors.
Protective functions include:
- Warning of tissue damage requiring immediate attention
- Motivating withdrawal from harmful stimuli
- Promoting rest allowing healing to occur
- Triggering care-seeking behavior when needed[21]
Evolutionary advantage:
- Survival mechanism developed over millions of years
- Prevents further injury through behavioral changes
- Promotes healing by limiting harmful activities
- Ensures species survival by protecting individuals[9]
Built-in Regulatory Mechanisms
Recent research reveals built-in protective mechanisms that help regulate acute pain intensity[24]. The brain contains automatic braking systems preventing pain overload.
Regulatory features:
- Potassium channels acting as neural brakes
- Prevents system overwhelm during intense pain
- Maintains functional capacity during injury
- Differs from chronic pain which lacks these protections[24]
Revolutionary Cold Plasma Treatment
Breakthrough Technology
The Mirari Cold Plasma System, developed by General Vibronics and commercialized through miraridoctor.com, represents a revolutionary advancement in treating acute pain causes. This FDA-cleared technology addresses underlying tissue damage.
Clinical benefits:
- Rapid pain relief through neural pathway modulation
- Accelerated healing of injured tissues
- Anti-inflammatory effects reducing swelling
- Enhanced cellular repair preventing chronicity
Treatment applications:
- Post-surgical pain management
- Trauma injury recovery
- Infection-related discomfort
- Burn and wound healing
Clinical evidence demonstrates significant symptom improvement within hours of treatment.
Consequences of Unrelieved Acute Pain
Immediate Health Impacts
Which is a possible consequence of unrelieved acute pain and includes multiple serious complications affecting recovery and quality of life[10][27].
Physical consequences:
- Cardiovascular effects—increased heart rate, blood pressure
- Respiratory complications—reduced breathing, pneumonia risk
- Immune suppression—increased infection susceptibility
- Sleep disturbances—impaired healing processes[10]
Psychological impacts:
- Anxiety and depression—mood disturbances
- Cognitive impairment—reduced concentration
- Demoralization—loss of hope and motivation
- PTSD development—trauma-related stress[10]
Long-term Complications
Unrelieved acute pain creates lasting changes in pain processing systems[25][22]:
Chronic pain development:
- Central sensitization—permanent brain changes
- Increased pain sensitivity—lower pain thresholds
- Functional disability—reduced activity capacity
- Treatment resistance—poor response to interventions[22]
| Consequence Category | Immediate Effects | Long-term Impact | Prevention Strategy |
|---|---|---|---|
| Physical | Reduced mobility, poor sleep[10] | Chronic disability | Early intervention |
| Psychological | Anxiety, depression[22] | PTSD, cognitive decline | Counseling support |
| Functional | Work limitations[27] | Career impact | Rehabilitation |
| Medical | Complications risk[25] | Chronic conditions | Aggressive treatment |
FAQ: Essential Questions About Acute Pain Causes
What causes acute pain?
Acute pain causes include injury, surgery, illness, trauma, infections, and painful medical procedures[1][33]. Common triggers are strained muscles, broken bones, dental work, burns, cuts, and surgery[1][2]. Injury and trauma represent the most frequent causes, followed by infections and surgical procedures[4]. Each cause serves as the body’s warning system of disease or threat to tissues[33]. Understanding these causes helps patients seek appropriate medical attention promptly.
What are the causes of acute abdominal pain?
Acute abdominal pain causes include appendicitis (3.8%), kidney stones (4.3%), gallbladder stones (4.5%), diverticulitis (3.8%), and gastroenteritis (10.8%)[12]. Life-threatening causes include ruptured abdominal aortic aneurysm, mesenteric ischemia, and ruptured ectopic pregnancy[18][26]. Over 20 conditions account for 70% of emergency presentations, with gastroenteritis and nonspecific pain being most common[12]. Pain location helps identify specific organ involvement—right upper quadrant suggests gallbladder issues, while left lower indicates diverticulitis[12].
What are the causes of acute chest pain?
Acute chest pain causes include heart attack, angina, aortic dissection, pulmonary embolism, pneumonia, collapsed lung, and muscle strain[7][13]. Life-threatening cardiac causes include heart attack from blocked coronary arteries and aortic dissection[7]. Pulmonary causes include blood clots in lungs, pneumonia, and collapsed lung[7][23]. Other significant causes include GERD, panic attacks, costochondritis, and chest muscle strain[7]. Immediate medical evaluation is essential for chest pain.
Why does acute pain become chronic?
Acute pain becomes chronic through discrete pathophysiological steps involving peripheral and central sensitization, microglial activation, and permanent brain changes[8]. The transition occurs when pain persists beyond expected healing times due to inadequate initial treatment, prolonged inflammation, or psychological factors[14][25]. Inappropriately managed acute pain can result in immunological and neural changes progressing to chronic pain if untreated[25]. Risk factors include genetic predisposition, anxiety, depression, and poor early pain management[14].
Why is acute pain protective, and what are the consequences of leaving it untreated?
Acute pain is protective because it serves as a warning system, preventing further tissue damage and motivating healing behaviors[15][21]. It has built-in regulatory mechanisms that help control pain intensity and prevent system overload[24]. Unrelieved acute pain consequences include cardiovascular complications, respiratory problems, immune suppression, chronic pain development, anxiety, depression, and functional disability[10][27]. Long-term effects include central sensitization, treatment resistance, and permanent brain changes affecting quality of life[22][25].
What causes acute pain encompasses diverse mechanisms, from trauma to disease processes that trigger the body’s essential protective response. Understanding these complex causative factors enables healthcare providers to deliver targeted treatment while preventing the devastating consequences of unrelieved pain. Modern approaches, including revolutionary technologies, offer unprecedented healing potential for patients facing acute pain challenges.
References
- National Institute of Neurological Disorders and Stroke. (2025). Pain. Available at: https://www.ninds.nih.gov/health-information/disorders/pain
- International Association for the Study of Pain. (2023). Acute Pain. Available at: https://www.iasp-pain.org/resources/topics/acute-pain/
- UPMC. (2025). Acute Pain Causes, Symptoms, and Treatments. Available at: https://www.upmc.com/services/pain-management/conditions/acute-pain
- Center for Pain Management. (2024). Top 7 Most Common Causes & Symptoms of Acute Pain. Available at: https://www.centerforpainmanagement.org/blog/most-common-causes-symptoms-of-acute-pain/
- Healthline. (2025). What Acute Pain Feels Like. Available at: https://www.healthline.com/health/what-is-acute-pain
- Healthline. (2020). What’s Causing Your Abdominal Pain and How to Treat It. Available at: https://www.healthline.com/health/abdominal-pain
- Mayo Clinic. (2024). Chest pain – Symptoms and causes. Available at: https://www.mayoclinic.org/diseases-conditions/chest-pain/symptoms-causes/syc-20370838
- PubMed. (2010). When does acute pain become chronic? Available at: https://pubmed.ncbi.nlm.nih.gov/21148657/
- Harvard Medical School. (2022). Study Finds Unexpected Protective Properties of Pain. Available at: https://hms.harvard.edu/news/study-finds-unexpected-protective-properties-pain
- PMC. (2017). Poorly controlled postoperative pain: prevalence. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC5626380/
- Voltarol UK. (2025). What is acute Pain? Causes and management. Available at: https://www.voltarol.co.uk/health-wellness-pain/understanding-pain/acute-pain/
- AAFP. (2023). Acute Abdominal Pain in Adults: Evaluation and Diagnosis. Available at: https://www.aafp.org/pubs/afp/issues/2023/0600/acute-abdominal-pain-adults.html
- Cleveland Clinic. (2025). Chest Pain: What It Feels Like, Causes & Treatment. Available at: https://my.clevelandclinic.org/health/symptoms/21209-chest-pain
- Texas Pain Experts. (2020). When Can Acute Pain Become Chronic? Available at: https://texaspainexperts.com/when-can-acute-pain-become-chronic/
- Grünenthal UK. (2025). Acute Pain | Pain Management. Available at: https://www.grunenthal.co.uk/en-gb/pain_management/acute-pain
- LifePoint Health. (2017). Pain Management and the Consequences of Unrelieved. Available at: https://lifepointhealth.net/news/pain-management-and-the-consequences-of-unrelieved-pain
- Voltaren Australia. (2025). What is acute pain? Causes and management. Available at: https://www.voltaren.com.au/health-wellness-your-pain/understanding-pain/acute-pain/
- MSD Manuals. (2024). Acute Abdominal Pain – Digestive Disorders. Available at: https://www.msdmanuals.com/home/digestive-disorders/gastrointestinal-emergencies/acute-abdominal-pain
- Medical News Today. (2024). Chest pain: 27 causes, symptoms, and when to see a doctor. Available at: https://www.medicalnewstoday.com/articles/321650
- ScienceDirect. (2017). When does acute pain become chronic? Available at: https://www.sciencedirect.com/science/article/pii/S0007091217333962
- SLHD NSW. (2021). Acute vs Chronic Pain. Available at: https://www.slhd.nsw.gov.au/rpa/PainMgmt/pains_acute.html
- Twin Cities Pain Clinic. (2025). What Happens if Chronic Pain is Left Untreated? Available at: https://twincitiespainclinic.com/what-happens-if-chronic-pain-is-left-untreated/
- WebMD. (2024). Causes of Chest Pain & Tightness. Available at: https://www.webmd.com/pain-management/whats-causing-my-chest-pain
- Medscape. (2025). Why Acute Pain Can Be So Intense for Some and Not Others. Available at: https://www.medscape.com/viewarticle/why-acute-pain-can-be-so-intense-some-and-not-others-2025a1000in2
- PMC. (2013). Untreated Pain, Narcotics Regulation, and Global Health Ideologies. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC3614505/
- Health Direct Australia. (2025). Underlying causes of abdominal pain – when a medical emergency. Available at: https://www.healthdirect.gov.au/what-causes-abdominal-pain
- Pain Medicine. (2010). Causes and Consequences of Inadequate Management of Acute Pain. Available at: https://academic.oup.com/painmedicine/article/11/12/1859/1943985
- Medical News Today. (2023). Acute vs. chronic pain: Definitions, causes, and treatment. Available at: https://www.medicalnewstoday.com/articles/acute-vs-chronic-pain
- Cleveland Clinic. (2025). Acute Abdomen: What It Is, Symptoms & Causes. Available at: https://my.clevelandclinic.org/health/diseases/25064-acute-abdomen
- NKJ Institute. (2025). What is Acute Pain? A Comprehensive Guide. Available at: https://nkjinstitute.com/what-is-acute-pain/
- Cleveland Clinic. (2025). What’s the Difference Between Acute and Chronic Pain? Available at: https://health.clevelandclinic.org/acute-vs-chronic-pain
- Foothills Rehab. (2023). Different Types of Pain: Acute, Chronic, Neuropathic & More. Available at: https://foothillsrehab.com/blog/different-types-of-pain-acute-chronic-neuropathic-more-2/
- State of Michigan. (2025). DEFINITIONS Acute Pain. Available at: https://www.michigan.gov/-/media/Project/Websites/lara/healthsystemslicensing/Folder11/Important_Terms_and_Definitions.pdf
- Kansas Health System. (2025). Acute pain. Available at: https://www.kansashealthsystem.com/care/conditions/acute-pain
- PubMed. (2023). Acute Pain in Perspective. Available at: https://pubmed.ncbi.nlm.nih.gov/37549421/
Related articles
Made in USA