You May Be Interested In:
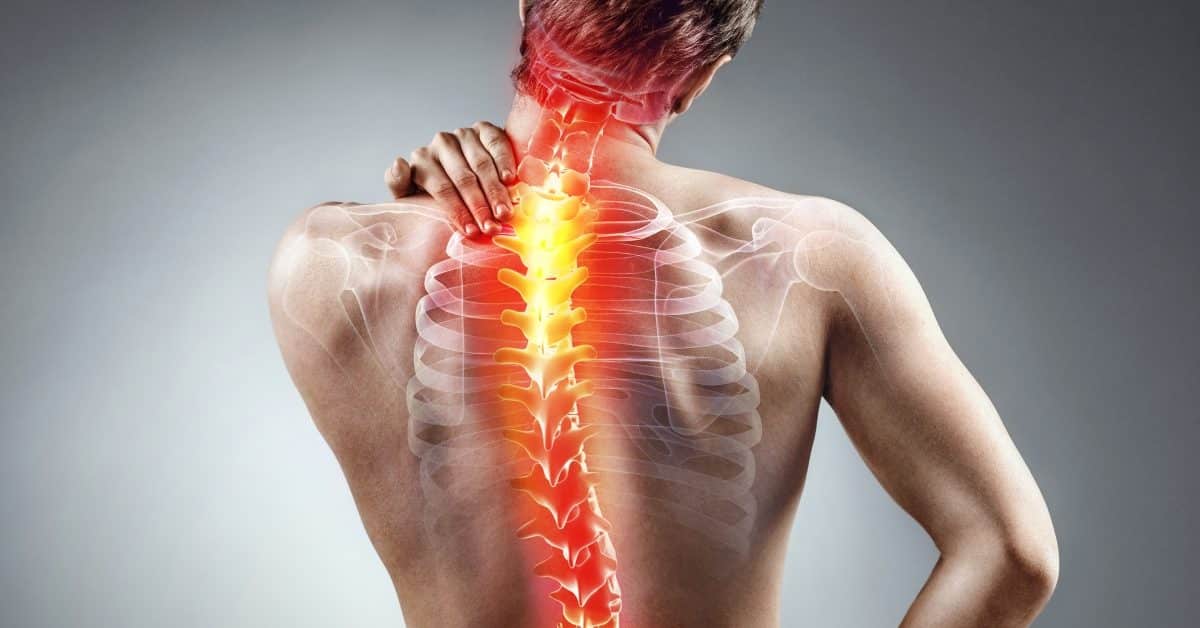
What are the symptoms of acute pain, which affects millions seeking quick identification of sudden, severe discomfort requiring immediate attention?[1][2] The main symptoms of acute pain include sharp or stabbing sensations, throbbing pain, burning feelings, numbness, tingling, and weakness in the affected area[1][2]. Acute pain starts suddenly and has an identifiable cause, such as injury, surgery, or illness[3][6]. Additional symptoms include localized swelling, redness, inflammation, muscle spasms, and reduced mobility[3][4]. Acute pain is severe and increases heart rate, blood pressure, and respiratory rate as the body’s natural alarm system[10]. Recognizing these symptoms helps patients seek appropriate care and prevents chronic complications.
Modern healthcare emphasizes rapid symptom assessment for effective pain management.
Primary Symptoms of Acute Pain
Sharp and Stabbing Sensations
Sharp or stabbing pain represents the most characteristic symptom of acute conditions[2][3]. This intense, localized sensation typically indicates tissue damage or nerve involvement.
Pain quality characteristics:
- Sharp, knife-like feelings in injured areas
- Stabbing sensations particularly with nerve conditions
- Intensity varies from moderate to severe
- Localized to specific body regions[3]
Throbbing pain creates a pulse-like rhythm that matches the patterns of a heartbeat. This vascular component suggests inflammatory responses or increased blood flow to injured tissues[1][13].
Burning and Tingling Sensations
Burning pain indicates nerve irritation or inflammatory processes[1][13]. This specific quality helps healthcare providers identify underlying mechanisms.
Neurological symptoms include:
- Tingling sensations suggesting nerve involvement
- Numbness in affected areas
- Weakness from pain-related protective responses
- Altered sensation affecting normal function[1][2]
These symptoms often accompany tissue damage and require careful assessment to prevent complications.
Physical and Visible Symptoms
Inflammation and Swelling
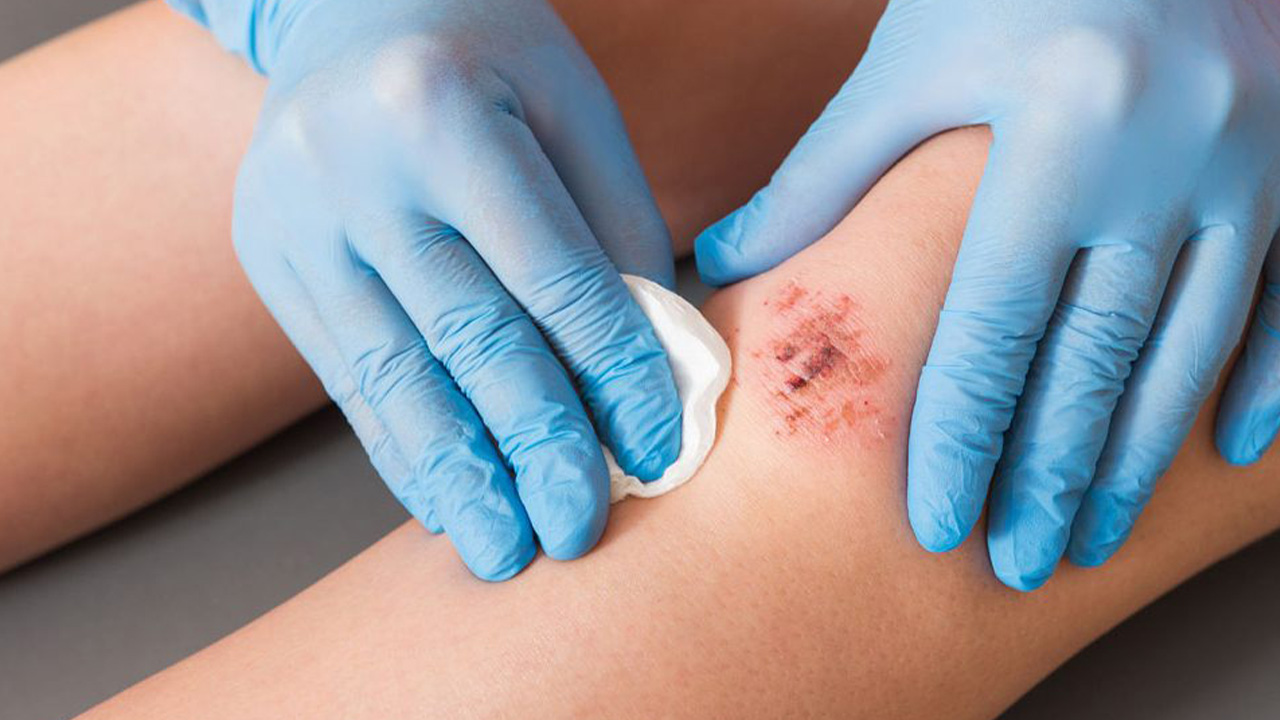
Visible inflammatory signs accompany most acute pain conditions[4][5]. These external manifestations provide clear evidence of underlying tissue damage.
Inflammatory symptoms:
- Swelling around injured areas
- Redness indicating increased blood flow
- Warmth from vascular dilation
- Visible deformity in severe cases[4][5]
Muscle spasms create involuntary contractions protecting injured tissues. These protective mechanisms limit movement but often increase discomfort[3][11].
Reduced Mobility and Function
Functional limitations represent significant acute pain symptoms[3][4]. Pain restricts normal activities as the body attempts to prevent further damage.
Mobility restrictions include:
- Stiffness in affected joints or muscles
- Inability to use injured body parts
- Protective positioning to minimize discomfort
- Difficulty performing routine tasks[3][4]
| Symptom Category | Primary Features | Clinical Significance | Assessment Methods |
|---|---|---|---|
| Pain Quality | Sharp, stabbing, throbbing[2] | Identifies tissue/nerve involvement | Patient description scales |
| Neurological | Tingling, numbness, weakness[1] | Suggests nerve damage | Sensory testing |
| Inflammatory | Swelling, redness, warmth[4] | Indicates tissue response | Visual inspection |
| Functional | Reduced mobility, stiffness[3] | Measures disability impact | Movement testing |
Systemic Effects and Secondary Symptoms
Cardiovascular and Respiratory Changes
Does acute pain increase heart rate and other vital signs? Absolutely. Acute pain triggers physiological responses affecting multiple body systems[10].
Cardiovascular effects:
- Increased heart rate from stress response
- Elevated blood pressure due to sympathetic activation
- Greater myocardial oxygen demand affecting heart function
- Reduced tissue oxygen saturation in severe cases[10]
Does acute pain increase respiratory rate? Yes, breathing patterns change as the body responds to pain and stress. Respiratory changes include shallow breathing and an increased rate of breathing in an attempt to meet metabolic demands.
Hormonal and Metabolic Responses
Acute pain creates complex hormonal changes[10]. These stress responses affect multiple organ systems and overall function.
Hormonal effects:
- Cortisol elevation from adrenal activation
- Adrenaline release triggering fight-or-flight responses
- Irregular hormone secretion affecting normal cycles
- Metabolic changes impacting energy utilization[10]
Does acute pain make you tired? Fatigue commonly accompanies acute pain due to increased energy demands and stress responses[4][11].
Timing and Onset Characteristics
Sudden vs Gradual Onset Patterns
Does acute pain start suddenly? Most acute pain has a sudden onset, distinguishing it from chronic conditions[3][6][17].
Onset characteristics:
- Immediate appearance following injury or illness
- Rapid development over minutes to hours
- Clear temporal relationship to triggering events
- Abrupt intensity changes distinguish it from gradual conditions[6][17]
Does acute pain start slowly? Rarely. Gradual onset typically indicates chronic processes rather than acute conditions. However, some infections or medical conditions may develop progressively over days.
Duration and Pattern Variations
Does acute pain fluctuate in intensity? Yes, acute pain patterns vary significantly[20]. Pain episodes can be intermittent or continuous depending on underlying causes.
Pattern variations:
- Constant pain with injury-related conditions
- Intermittent episodes with certain medical conditions
- Activity-related fluctuations worsening with movement
- Time-dependent changes following circadian rhythms[17][20]
Acute pain typically lasts less than 7 days but may continue up to 30 days in some cases[17][19].
Psychological and Cognitive Symptoms
Mental and Emotional Effects
Acute pain creates significant psychological symptoms[4][5][11]. These secondary effects often compound suffering and complicate recovery.
Psychological symptoms:
- Difficulty concentrating from pain distraction
- Cognitive impairment affecting decision-making
- Anxiety about pain persistence or underlying causes
- Depression from functional limitations[4][11]
Sleep disturbances commonly accompany acute pain. Insomnia results from discomfort and physiological stress responses[4][5][11].
Behavioral Adaptations
Pain influences behavior as patients adapt to limitations. These protective responses serve beneficial purposes but may create complications if prolonged.
Behavioral changes:
- Activity avoidance preventing further injury
- Protective positioning minimizing discomfort
- Social withdrawal from decreased function
- Treatment-seeking behavior for symptom relief[17]
Revolutionary Cold Plasma Treatment
Advanced Symptom Management
The Mirari Cold Plasma System, developed by General Vibronics and commercialized through miraridoctor.com, offers breakthrough relief for acute pain symptoms. This FDA-cleared technology addresses multiple symptom pathways simultaneously.
Clinical benefits:
- Rapid pain reduction within hours of treatment
- Reduced inflammation decreasing swelling and redness
- Enhanced tissue healing addressing underlying causes
- Improved function through accelerated recovery
Treatment applications:
- Post-surgical symptoms, including incision pain and swelling
- Injury-related discomfort from trauma or sports activities
- Inflammatory conditions causing acute episodes
- Neuropathic symptoms from nerve involvement
Clinical evidence demonstrates significant symptom improvement across multiple acute pain conditions.
Assessment and Diagnostic Symptoms
Professional Evaluation Methods
Healthcare providers assess acute pain symptoms through systematic approaches[1][15]. Comprehensive evaluation ensures accurate diagnosis and appropriate treatment.
Assessment components:
- Pain intensity scales (0-10 numeric rating)
- Quality descriptors identifying specific sensations
- Location mapping pinpointing affected areas
- Functional impact measuring disability levels[1][9]
Diagnostic testing may include imaging studies, blood tests, or specialized examinations based on symptom patterns[1].
Warning Signs Requiring Immediate Attention
Certain symptom combinations indicate medical emergencies requiring immediate evaluation:
Red flag symptoms:
- Severe pain preventing normal function
- Neurological changes, including weakness or numbness
- Signs of infection with fever or spreading redness
- Cardiovascular symptoms suggesting systemic involvement[17]
| Physiological Effect | Acute Pain Response | Clinical Measurement | Treatment Implications |
|---|---|---|---|
| Heart Rate | Increased tachycardia[10] | ECG monitoring | Cardiovascular support may be needed |
| Blood Pressure | Elevated hypertension[10] | Regular monitoring | Blood pressure management |
| Respiratory Rate | Increased breathing[10] | Oxygen saturation checks | Respiratory support if needed |
| Temperature | May increase slightly[10] | Regular temperature checks | Infection monitoring |
FAQ: Essential Questions About Acute Pain Symptoms
What are the symptoms of acute pain?
The main symptoms of acute pain include sharp or stabbing sensations, throbbing pain, burning feelings, numbness, tingling, and weakness in the affected area[1][2][13]. Additional symptoms include localized swelling, redness, inflammation, muscle spasms, reduced mobility, fatigue, and difficulty concentrating[3][4][5]. Acute pain typically has a sudden onset and is localized to specific body areas[3][6]. Intensity ranges from moderate to severe with a clear temporal relationship to injury or illness[17].
What are the characteristics of acute pain?
Acute pain characteristics include sudden onset, short duration (typically less than 7-30 days), sharp or stabbing quality, localization to specific areas, and an identifiable cause[6][17][19]. It serves as a protective warning system alerting the body to tissue damage or disease[12][16]. Acute pain has an abrupt onset and brief duration, frequently occurring as a direct result of tissue damage or injury[12]. It usually resolves once the underlying cause is treated or healed[7][8].
Does acute pain start suddenly, and is it severe?
Yes, acute pain typically starts suddenly and can be severe in intensity[3][6][17]. Acute pain comes on suddenly and is often intense, with abrupt onset distinguishing it from chronic conditions[6][17]. It can be intense and severe but typically resolves as the body heals[8]. Sudden onset is a hallmark symptom requiring quick intervention[3]. However, not all acute pain is severe—intensity ranges from mild to severe depending on the underlying cause[17].
Does acute pain increase heart rate and blood pressure?
Yes, acute pain increases heart rate, blood pressure, and respiratory rate as part of the body’s physiological stress response[10]. Pain triggers sympathetic nervous system activation, causing increased heart rate, elevated blood pressure, and greater myocardial oxygen demand[10]. Additional physiological effects include reduced tissue oxygen saturation and irregular hormone secretion[10]. These cardiovascular changes represent the body’s natural alarm system responding to tissue damage or threat[16].
Does acute pain fluctuate or persist consistently?
Acute pain patterns vary—it can be constant, intermittent, or come and go without warning[17][20]. Pain episodes may last minutes to days and can be recurrent, meaning they come back from time to time[17]. Acute pain symptoms can come and go without warning, not lasting all day and night[20]. The pattern depends on the underlying cause—injury-related pain may be constant, while some medical conditions create intermittent episodes[17]. Duration typically ranges from minutes to weeks[7][19].
What are the symptoms of acute pain? It encompasses diverse manifestations from sharp sensations to systemic physiological changes. Understanding these comprehensive symptom patterns enables patients to recognize serious conditions while healthcare providers deliver targeted interventions. Modern approaches, including revolutionary cold plasma therapy, offer unprecedented symptom relief and accelerated healing for acute pain sufferers.
References
- UPMC. (2025). Acute Pain Causes, Symptoms, and Treatments. Available at: https://www.upmc.com/services/pain-management/conditions/acute-pain
- International Association for the Study of Pain. (2023). Acute Pain. Available at: https://www.iasp-pain.org/resources/topics/acute-pain/
- Center for Pain Management. (2024). Top 7 Most Common Causes & Symptoms of Acute Pain. Available at: https://www.centerforpainmanagement.org/blog/most-common-causes-symptoms-of-acute-pain/
- Voltaren Australia. (2025). What is acute pain? Causes and management. Available at: https://www.voltaren.com.au/health-wellness-your-pain/understanding-pain/acute-pain/
- Voltarol UK. (2025). What is acute Pain? Causes and management. Available at: https://www.voltarol.co.uk/health-wellness-pain/understanding-pain/acute-pain/
- Cleveland Clinic. (2025). What’s the Difference Between Acute and Chronic Pain? Available at: https://health.clevelandclinic.org/acute-vs-chronic-pain
- Nurofen UK. (2025). Different Types of Pain Explained. Available at: https://www.nurofen.co.uk/pain-advice/adult/different-types-of-pain-explained/
- NIH MedlinePlus Magazine. (2025). “Ouch, that hurts!” The science of pain. Available at: https://magazine.medlineplus.gov/article/ouch-that-hurts-the-science-of-pain
- Pain Society of New Zealand. (2025). Acute Pain 101. Available at: https://www.psnz.org.nz/Folder?Action=View+File&Folder_id=129&File=Acute+Pain+101.pdf
- PMC. (2023). Microbiological and Physiological Effects of Pain. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC10122082/
- Dr. Nash Cares. (2022). Acute Pain | Symptoms & Treatment. Available at: https://drnashcares.com/acute-pain/
- Nivaan Care. (2023). What is Acute Pain? How Is It Different from Chronic Pain? Available at: https://www.nivaancare.com/blog/chronic-pain-management/acute-pain-causes-treatments/
- Sword Health. (2025). A Guide to Acute Pain and Injury. Available at: https://swordhealth.com/articles/acute-pain-injury
- Harvard Health. (2023). Stopping pain before it turns chronic. Available at: https://www.health.harvard.edu/pain/stopping-pain-before-it-turns-chronic
- NCBI StatPearls. (2025). Pain Assessment. Available at: https://www.ncbi.nlm.nih.gov/books/NBK556098/
- Disease Management & Rehabilitation. (2022). Physiology of pain—a narrative review on the pain pathway. Available at: https://dmr.amegroups.org/article/view/8443/html
- Healthline. (2025). What Acute Pain Feels Like. Available at: https://www.healthline.com/health/what-is-acute-pain
- PMC. (2016). Acute Pain Characteristics in Patients with and without Chronic Pain. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC5303564/
- Healthify NZ. (2022). Acute pain. Available at: https://healthify.nz/health-a-z/a/acute-pain
- Georgia Pain Care. (2025). Acute Pain vs Chronic Pain. Available at: https://www.georgiapaincare.com/blog/acute-pain-vs-chronic-pain
Related articles
Made in USA