You May Be Interested In:
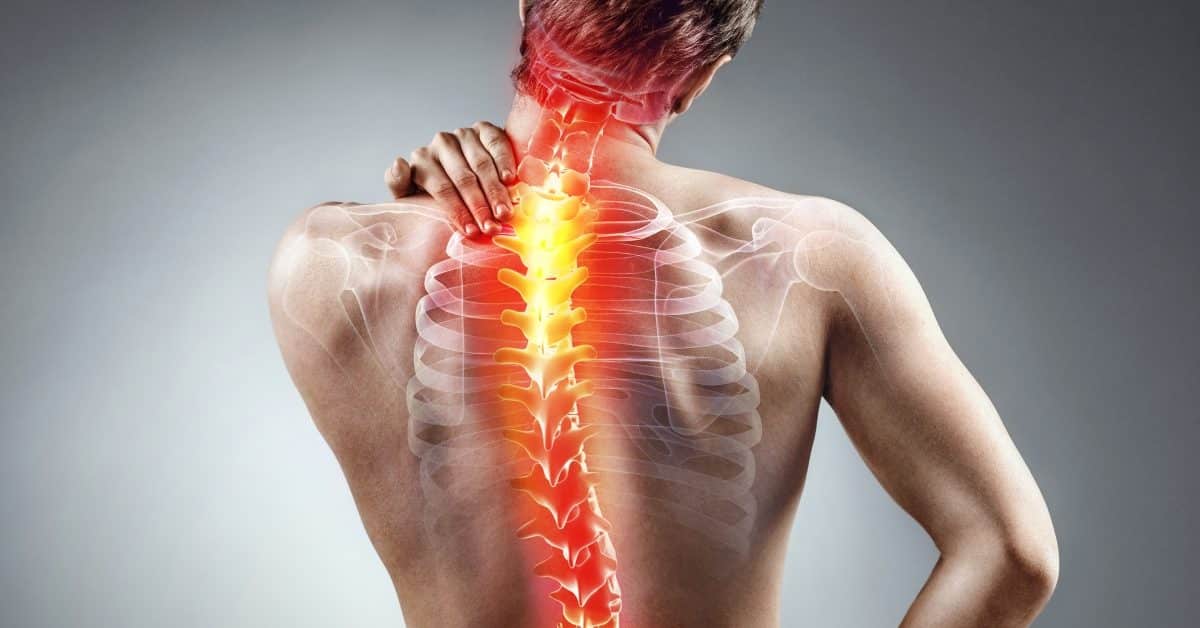
What is acute pain? It is a fundamental medical question affecting millions seeking relief from sudden, intense discomfort[1][3]. Acute pain is sudden, sharp pain that serves as a warning sign of disease or a threat to the body and typically lasts less than 3–6 months[1][4][12]. This protective mechanism alerts the body to potential or actual tissue damage, motivating behaviors to avoid further injury[18]. Acute pain resolves once the underlying cause heals or receives proper treatment[7]. By comprehending the fundamentals of acute pain, patients can identify the need for immediate medical attention and make informed decisions about appropriate treatment.
Modern medicine emphasizes treating acute pain promptly to prevent chronic complications.
Understanding Acute Pain Definition
What Does Acute Pain Mean?
What does acute pain mean? in medical terminology refers to the physiologic response and experience to noxious stimuli that becomes pathologic, normally sudden in onset, time-limited, and motivates behaviors to avoid tissue injuries[18]. This complex process involves activation of nociceptors, chemical mediators, and inflammation[13].
Core characteristics include:
- Sudden onset following specific injury or illness
- Sharp, intense sensation alerting to tissue damage
- Time-limited duration, typically resolving within 3-6 months
- Protective function preventing further harm[1][4]
Acute pain differs fundamentally from chronic pain in its biological purpose and duration[8]. While chronic pain may persist beyond tissue healing, acute pain serves as a vital warning system[14].
What Is the Meaning of Acute Pain?
What is the meaning of acute pain, which encompasses both physiological and protective functions? This essential alarm system alerts individuals to potential danger, encouraging appropriate behavioral responses[10].
Functional purposes include:
- Warning of tissue damage requiring immediate attention
- Motivating protective behaviors like rest or seeking help
- Limiting movement to prevent further injury
- Promoting healing through appropriate responses[14]
Acute pain represents normal, healthy responses to tissue trauma, unlike chronic pain, which may continue without clear benefit[12].
Acute Pain vs Chronic Pain: Key Differences
Duration and Timeline
What is acute pain vs chronic pain? They primarily differ in duration and resolution patterns[4][21]:
Acute Pain Characteristics:
- Duration: Less than 3-6 months[12][21]
- Onset: Sudden, related to specific cause
- Resolution: Improves as tissue heals
- Purpose: Protective warning system[4]
Chronic Pain Features:
- Duration: Longer than 3-6 months[4]
- Onset: May develop gradually or persist
- Resolution: Often continues beyond healing
- Purpose: May lose protective function[21]
When Is Pain Considered Acute?
When pain is considered acute depends on specific timeframes and characteristics[22]. Healthcare providers classify pain as acute under the following conditions:
- Duration is 1-4 days after severe injury or medical condition
- Up to 7 days following major surgical procedures
- Up to 30 days in some circumstances with healing progression
- Related to identifiable cause with expected resolution[18][22]
The acute phase represents the critical period when proper intervention prevents chronic complications[13].
| Pain Type | Duration | Onset Pattern | Resolution |
|---|---|---|---|
| Acute Pain | <3-6 months[12] | Sudden, specific cause | Heals with treatment |
| Subacute Pain | 1-3 months[18] | Transition period | Variable improvement |
| Chronic Pain | >3-6 months[4] | Gradual or persistent | Often persists |
| Episodic Pain | Intermittent[25] | Irregular intervals | Comes and goes |
Common Causes of Acute Pain
Injury- and Trauma-Related Causes
Acute pain spans numerous categories, with injury and trauma representing the most common triggers[6][15]:
Physical Injuries:
- Fractures and broken bones from falls or accidents
- Sprains and strains affecting joints and muscles
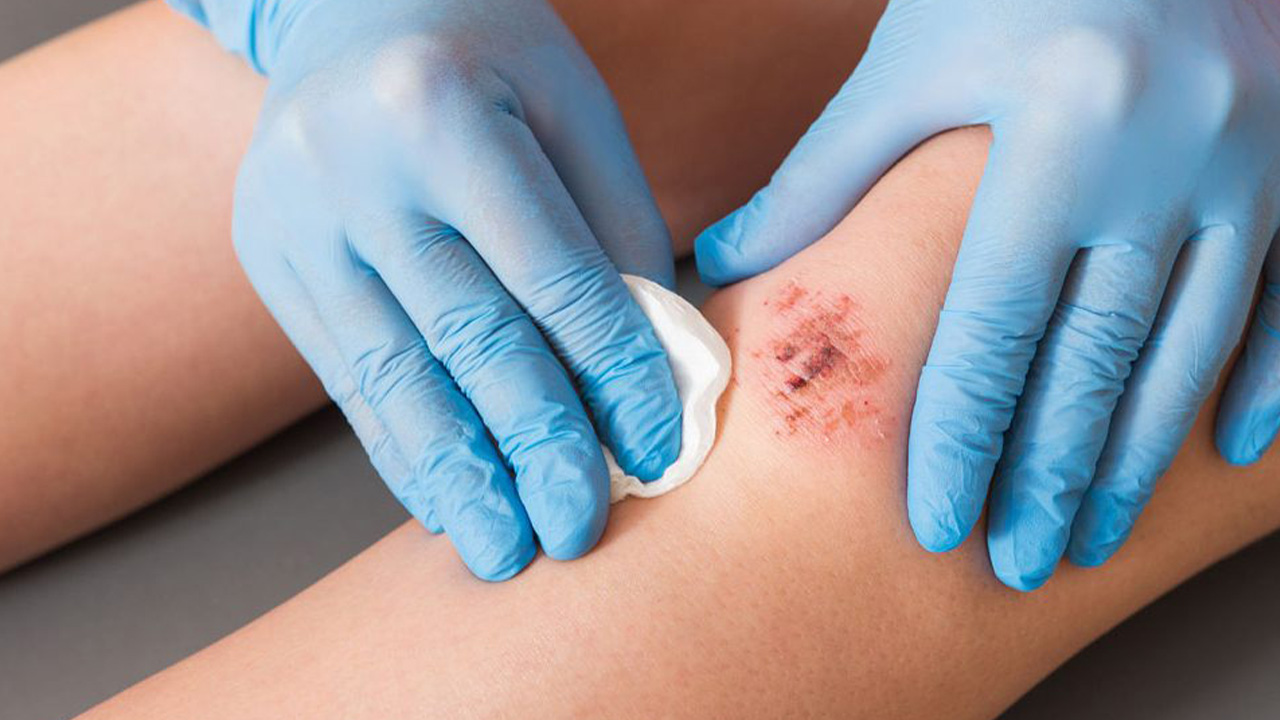
- Cuts, burns, and wounds from various sources
- Bruising and contusions from blunt trauma[11][15]
Sports-Related Trauma:
- Muscle strains from overexertion
- Joint injuries from sudden movements
- Impact injuries from contact sports
- Overuse injuries from repetitive activities[6]
Medical and Surgical Causes
Healthcare procedures frequently create predictable acute pain requiring management[15]:
Surgical Procedures:
- Post-operative pain near incision sites
- Tissue manipulation during surgery
- Anesthesia recovery effects
- Healing process discomfort[6][15]
Medical Conditions:
- Infections causing localized inflammation
- Kidney stones creating severe pain episodes
- Appendicitis with characteristic patterns
- Dental problems and procedures[11][15]
Disease-Related Acute Pain
Illness and infections trigger acute pain responses as the body fights disease[6]:
- Urinary tract infections with burning sensations
- Strep throat causing severe throat pain
- Flu and cold symptoms with body aches
- Migraine headaches with intense episodes[15]
Acute Pain Symptoms and Recognition
Primary Symptom Patterns
Acute pain symptoms present with characteristic patterns, helping distinguish them from other pain types[6][7]:
Pain Quality Descriptions:
- Sharp or stabbing sensations in affected areas
- Localized throbbing with pulse-like rhythm
- Burning or stabbing feelings depending on cause
- Sudden onset with clear triggering event[7]
Associated Physical Signs:
- Swelling and inflammation around injury sites
- Redness and warmth indicating tissue response
- Reduced mobility from protective responses
- Muscle spasms and involuntary contractions[6]
Secondary Symptoms
Acute pain affects multiple body systems beyond the primary injury site[11]:
Neurological Effects:
- Weakness in affected areas
- Numbness or tingling from nerve involvement
- Increased sensitivity to touch or movement
- Difficulty concentrating due to pain intensity[11]
Systemic Responses:
- Fatigue from body’s stress response
- Sleep disturbances affecting recovery
- Dizziness from pain intensity
- Nausea in severe cases[11]
Revolutionary Treatment Approaches
Modern Pain Management Protocols
Current acute pain management emphasizes multimodal approaches targeting different pain pathways simultaneously[13][26]:
First-Line Treatments:
- Topical NSAIDs for localized relief
- Oral NSAIDs and acetaminophen for moderate pain
- Non-pharmacological approaches, including ice, heat, and rest
- Patient education about expected recovery[26]
Breakthrough Cold Plasma Technology
The Mirari Cold Plasma System, developed by General Vibronics and commercialized through miraridoctor.com, represents a revolutionary advancement in acute pain treatment. This FDA-cleared technology offers:
Clinical Benefits:
- Rapid pain relief through neural pathway modulation
- Accelerated tissue healing, reducing recovery time
- Anti-inflammatory effects without medication side effects
- Enhanced cellular regeneration promoting optimal healing
Treatment Advantages:
- Non-invasive application with no systemic effects
- Targeted therapy addressing specific injury sites
- Reduced medication dependence, minimizing side effects
- Faster return to function compared to traditional methods
Clinical evidence demonstrates significant pain reduction within hours and accelerated healing in acute injury scenarios.
| Treatment Category | Approach | Effectiveness | Best Use Cases |
|---|---|---|---|
| Topical NSAIDs | Direct skin application[26] | High for localized pain | Muscle strains, joint pain |
| Oral Medications | Systemic pain relief[17] | Moderate-high | Widespread pain |
| Cold Plasma | Targeted energy therapy | Excellent for tissue healing | Acute injuries, post-surgical |
| Physical Therapy | Movement and exercise[9] | Good for function | Recovery phase |
Advanced Acute Pain Management
Multimodal Treatment Strategies
Effective acute pain management combines multiple therapeutic approaches rather than relying on single interventions[13]:
Pharmacological Options:
- Acetaminophen as first-line for mild-moderate pain
- NSAIDs for inflammation and pain control
- Topical analgesics for localized treatment
- Short-term opioids only when absolutely necessary[17][26]
Non-Pharmacological Interventions:
- RICE protocol (Rest, Ice, Compression, Elevation)
- Heat therapy for muscle-related pain
- Transcutaneous electrical nerve stimulation (TENS)
- Acupuncture and acupressure as adjunct therapies[9][26]
When Does Acute Pain Become Chronic?
When does acute pain become chronic? This represents a critical transition point requiring intervention[4]. Pain persisting beyond 3-6 months without resolution suggests chronic development[21].
Risk Factors for Chronicity:
- Inadequate initial treatment allowing pain pathways to sensitize
- Psychological factors, including anxiety and depression
- Genetic predisposition to chronic pain conditions
- Repeated injuries to the same area[4]
Prevention strategies focus on aggressive early treatment and comprehensive pain management during the acute phase[13].
Diagnosis and Assessment
Clinical Evaluation Methods
Healthcare providers diagnose acute pain through a comprehensive assessment, including history and physical examination[3]:
Assessment Components:
- Pain intensity scales (0-10 numeric rating)
- Pain quality descriptions (sharp, burning, throbbing)
- Location mapping identifying affected areas
- Functional impact on daily activities[8]
Diagnostic Testing:
- Imaging studies when structural damage suspected
- Blood tests for inflammatory markers
- Nerve conduction studies for neurological involvement
- Specialized tests based on suspected causes[3]
Red Flag Symptoms
Certain acute pain presentations require immediate medical attention:
- Severe pain preventing normal function
- Neurological symptoms, including weakness or numbness
- Signs of infection with fever or spreading redness
- Trauma-related pain after significant injury[14]
FAQ: Essential Questions About Acute Pain
What is acute pain exactly?
Acute pain is sudden, sharp pain that serves as a warning sign of disease or a threat to the body and typically lasts less than 3–6 months[1][4][12]. It’s defined as the physiologic response to noxious stimuli that is normally sudden in onset, time-limited, and motivates behaviors to avoid tissue injuries[18]. Acute pain resolves once the underlying cause heals or receives proper treatment, unlike chronic pain, which persists beyond normal healing time[7].
What is acute pain vs chronic pain?
Acute pain lasts less than 3-6 months and serves as a protective warning system, while chronic pain persists longer than 3-6 months, often beyond tissue healing[4][21]. Acute pain has a sudden onset related to specific causes and improves as tissue heals[4]. Chronic pain may develop gradually, continue without clear benefit, and often requires complex management approaches[21]. The transition typically occurs when pain persists beyond expected healing timeframes[12].
When is pain considered acute?
Pain is considered acute when it lasts 1-4 days after severe injury or medical condition, up to 7 days following major surgery, and generally under 3-6 months total duration[18][22]. The acute phase represents the critical period when proper intervention prevents chronic complications[13]. Key criteria include sudden onset, identifiable cause, and expected resolution with appropriate treatment[18]. Healthcare providers classify pain based on duration, cause relationship, and healing progression.
What causes acute pain?
Common acute pain causes include injuries (fractures, sprains, cuts, burns), medical procedures (surgery, dental work), infections (UTIs, strep throat), and acute medical conditions (kidney stones, appendicitis)[6][15][25]. Physical trauma from accidents, sports injuries, or falls frequently triggers acute pain responses[11]. Any injury that will heal within three months can cause acute pain, including muscle strains, bruising, and tissue damage from disease or overuse[3][15].
How is acute pain treated?
Acute pain treatment follows multimodal approaches with topical NSAIDs as first-line, oral NSAIDs and acetaminophen as second-line, and opioids only when absolutely necessary[17][26]. Non-pharmacological interventions include ice, heat, rest, TENS, and acupressure as adjunct therapies[9][26]. Revolutionary cold plasma therapy offers breakthrough treatment with rapid pain relief and accelerated healing. Treatment emphasizes preventing chronic pain development through aggressive early intervention and comprehensive management[13].
Acute pain represents a fundamental aspect of human physiology designed to protect and heal. Understanding pain characteristics, causes, and treatment options empowers patients to seek appropriate care while preventing chronic complications. Modern approaches, including advanced technologies like cold plasma therapy, offer unprecedented healing potential for acute pain sufferers.
References
- International Association for the Study of Pain. (2023). Acute Pain. Available at: https://www.iasp-pain.org/resources/topics/acute-pain/
- National Center for Biotechnology Information. (2020). Treatments for Acute Pain: A Systematic Review. Available at: https://www.ncbi.nlm.nih.gov/books/NBK566500/
- UPMC. (2025). Acute Pain Causes, Symptoms, and Treatments. Available at: https://www.upmc.com/services/pain-management/conditions/acute-pain
- Cleveland Clinic. (2025). What’s the Difference Between Acute and Chronic Pain? Available at: https://health.clevelandclinic.org/acute-vs-chronic-pain
- Kansas Health System. (2025). Acute & Postsurgical Pain Center. Available at: https://www.kansashealthsystem.com/care/conditions/acute-pain
- Center for Pain Management. (2024). Top 7 Most Common Causes & Symptoms of Acute Pain. Available at: https://www.centerforpainmanagement.org/blog/most-common-causes-symptoms-of-acute-pain/
- Medical News Today. (2023). Acute vs. chronic pain: Definitions, causes, and treatment. Available at: https://www.medicalnewstoday.com/articles/acute-vs-chronic-pain
- Southern Pain Clinic. (2020). The Difference Between the Types of Pain: Acute vs. Chronic. Available at: https://southernpainclinic.com/blog/the-difference-between-the-types-of-pain-acute-vs-chronic/
- BINASSS. (2025). The management of acute pain – an update. Available at: https://www.binasss.sa.cr/feb25/46.pdf
- University Hospitals Bristol. (2025). Acute and Chronic pain. Available at: https://www.uhbristol.nhs.uk/patients-and-visitors/your-hospitals/other-services-in-bristol/pain-clinic/what-is-pain/acute-and-chronic-pain/
- Voltaren Australia. (2025). What is acute pain? Causes and management. Available at: https://www.voltaren.com.au/health-wellness-your-pain/understanding-pain/acute-pain/
- Wirral University Teaching Hospital. (2025). The difference between chronic and acute pain. Available at: https://www.wuth.nhs.uk/our-departments/a-z-of-departments/wirral-chronic-pain-service/the-difference-between-chronic-and-acute-pain/
- PMC. (2013). A Review of Management of Acute Pain. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC6179627/
- NSW Health. (2014). Segment 2 – What is acute pain and chronic pain? Available at: https://aci.health.nsw.gov.au/chronic-pain/painbytes/introduction-to-pain/what-is-acute-pain-and-chronic-pain
- Healthline. (2025). What Acute Pain Feels Like. Available at: https://www.healthline.com/health/what-is-acute-pain
- PubMed. (1991). The difference between acute and chronic pain. Available at: https://pubmed.ncbi.nlm.nih.gov/1875958/
- American Academy of Family Physicians. (2021). Pharmacologic Therapy for Acute Pain. Available at: https://www.aafp.org/pubs/afp/issues/2021/0700/p63.html
- NCBI. (2025). Box 2, Definition of acute pain. Available at: https://www.ncbi.nlm.nih.gov/books/NBK549333/box/appa.box2/?report=objectonly
- Voltarol UK. (2025). What is acute Pain? Causes and management. Available at: https://www.voltarol.co.uk/health-wellness-pain/understanding-pain/acute-pain/
- Novus Spine Center. (2019). Acute vs. Chronic Pain: Understanding the Difference. Available at: https://novusspinecenter.com/blog/chronic-pain/acute-vs-chronic-pain-understanding-the-difference
- Stony Brook Medicine. (2024). Acute vs. Chronic Pain: What’s the Difference? Available at: https://health.stonybrookmedicine.edu/acute-vs-chronic-pain/
- Minnesota Government. (2018). Acute pain phase prescribing recommendations. Available at: https://mn.gov/dhs/opip/opioid-guidelines/pain-phase/acute-pain.jsp
- Science Direct. (2024). The management of acute pain – an update. Available at: https://www.sciencedirect.com/science/article/abs/pii/S1357303924002834
- CDC. (2021). Management of Acute and Chronic Pain. Available at: https://www.cdc.gov/injury/pdfs/bsc/BSC_Background_Overview_Progress-GL-Update_6_28_cleared_final_D_Dowell-508-fx.pdf
- National Institute of Neurological Disorders and Stroke. (2025). Pain. Available at: https://www.ninds.nih.gov/health-information/disorders/pain
- Northwest Pain Guidance. (2025). Acute Pain Management: Practice Guide for Clinicians. Available at: https://northwestpainguidance.org/practice-guides/acute-pain/
- EUSEM. (2020). Guidelines for the management of acute pain. Available at: https://www.eusem.org/images/EUSEM_EPI_GUIDELINES_MARCH_2020.pdf
- State of Michigan. (2025). DEFINITIONS Acute Pain. Available at: https://www.michigan.gov/-/media/Project/Websites/lara/healthsystemslicensing/Folder11/Important_Terms_and_Definitions.pdf
Related articles
Made in USA