You May Be Interested In:
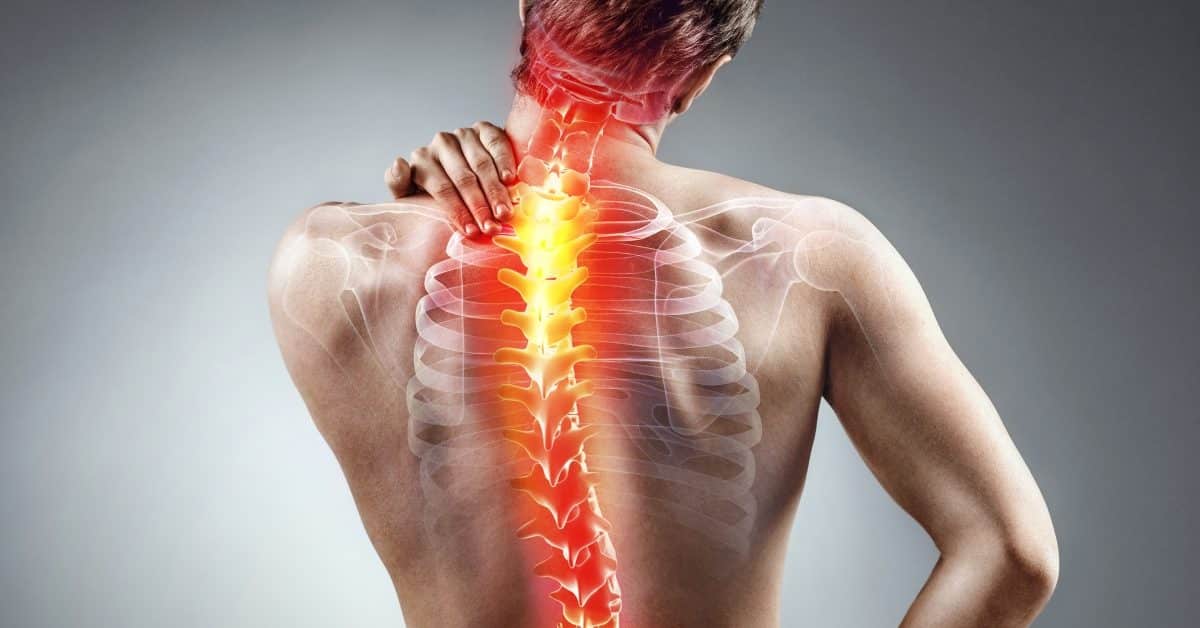
Can acute pain cause high blood pressure? Yes, acute pain can raise blood pressure temporarily through activation of the sympathetic nervous system[1][2]. Researchers have found a relationship between acute pain symptoms and high blood pressure, with low back pain and headache as the most common types[1]. Pain stimulates the sympathetic nervous system, triggering the fight-or-flight response that causes blood vessels to narrow and the heart to pump faster, resulting in elevated blood pressure[5]. Can acute pain raise blood pressure? Absolutely – once the pain subsides, blood pressure usually returns to normal, unlike chronic pain which can cause persistent hypertension[5][6]. Understanding these physiological responses helps patients recognize when acute pain symptoms require immediate medical attention.
The Physiology Behind Pain and Blood Pressure
How Acute Pain Triggers Blood Pressure Changes
Acute pain increases blood pressure by increasing sympathetic activity[6]. When your body experiences sudden pain, it activates a complex cascade of physiological responses designed to protect you from danger.
The sympathetic nervous system response includes:
- Blood vessel constriction reducing circulation to non-essential areas
- Increased heart rate pumping blood more rapidly
- Elevated stroke volume with each heartbeat
- Enhanced peripheral resistance throughout the circulatory system[17]
This fight-or-flight response evolved as survival mechanism allowing humans to escape immediate harm[14]. Direct effects include increased heart rate, stroke volume and peripheral resistance, which increase myocardial oxygen demand[17].
Acute vs Chronic Pain Effects
These relations are profoundly different in acute vs chronic pain[2]. While it’s widely recognized that pain can raise blood pressure acutely[2], the mechanisms differ significantly between short-term and long-term pain.
Key differences:
- Acute pain causes temporary spikes that resolve when pain subsides
- Chronic pain may lead to sustained hypertension over time
- Acute responses are protective and adaptive
- Chronic elevation becomes maladaptive and harmful[3]
Can Acute Pain Cause Nausea?
The Brain-Gut Connection
Can acute pain cause nausea? Yes, pain and digestion are closely linked in the brain, so feeling nauseous when you’re in pain isn’t unusual[7]. Pain signals are transmitted to the brain via nerves, which can trigger several physiological responses, including nausea[15].
Mechanisms include:
- Serotonin release in response to pain signals
- Cortisol production from stress hormone activation
- Disrupted digestive function from redirected blood flow
- Inflammatory chemical release affecting nausea centers[15]
Severe pain can directly lead to gastrointestinal distress through complex interactions between the nervous, immune, and endocrine systems[7]. This process involves the brain-gut axis – a communication network between the central nervous system and digestive tract.
Nausea Triggers in Acute Pain
Muscle pain, sprains, and strains can sometimes cause nausea, even though the gut isn’t directly injured[7]. Blood flow is redirected away from the stomach, slowing digestion and potentially triggering nausea[7].
Contributing factors:
- Stress response activation disrupting normal gut function
- Inflammatory mediators like cytokines and prostaglandins
- Central nervous system amplification of pain signals
- Altered gut microbiome from pain-related stress[7]
| Acute Pain Effect | Mechanism | Timeframe | Reversibility |
|---|---|---|---|
| High Blood Pressure | Sympathetic activation[6] | Minutes to hours | Yes, when pain resolves |
| Nausea | Brain-gut axis disruption[7] | Minutes to hours | Yes, with pain relief |
| Heart Rate Changes | Fight-or-flight response[17] | Immediate | Yes, temporary effect |
| Stress Hormones | HPA axis activation[15] | Minutes to hours | Yes, normalizes quickly |
Life-Threatening Complications
Can Acute Pain Kill You?
Can acute pain kill you? Yes, pain can kill through circulatory shock – a separate medical condition caused by acute, intense levels of pain[8][16]. When your body goes into shock, insufficient blood and oxygen reaches your cells, resulting in rapid and permanent tissue damage[8].
Critical mechanisms:
- Circulatory shock from severe pain overwhelming the system
- Insufficient oxygen reaching vital organs
- Rapid tissue damage if shock isn’t treated quickly
- Fatal organ damage including brain injury[16]
During wars, medics found that administering pain killers such as morphine to wounded soldiers and preventing them from going into shock could save their lives[8]. The quicker morphine was administered, the higher the survival rate[8].
Can Acute Pain Cause Heart Attack?
Can acute pain cause heart attack? People with chronic pain may be more likely to have a heart attack or stroke than those without chronic pain[9], but acute pain’s relationship is more complex.
Cardiovascular risks include:
- Increased myocardial oxygen demand from elevated heart rate
- Enhanced peripheral resistance stressing the heart
- Sympathetic overstimulation triggering arrhythmias
- Blood pressure spikes potentially rupturing vulnerable plaques[17]
Pain may trigger factors linked to poor heart health, including stress, reduced ability to exercise, poor sleep, and depression[9]. However, the immediate risk from acute pain is generally lower than chronic pain’s cumulative effects.
Can Acute Pain Be Neuropathic?
Understanding Acute Neuropathic Pain
Can acute pain be neuropathic? Yes, neuropathic pain can be a common symptom in acute and subacute peripheral neuropathies[10]. Acute neuropathic pain is a condition that is under-recognized, often difficult to treat and one that may progress to persistent pain and disability[18].
Characteristics of acute neuropathic pain:
- Results from damage to the nervous system rather than tissue injury
- Can occur suddenly following nerve trauma or disease
- Often described as burning, shooting, or electric shock-like
- May progress to chronic neuropathic pain without treatment[23]
In Guillain-Barré syndrome, the commonest cause of acute peripheral neuropathy, the pooled estimate of neuropathic pain was 34.8%[10]. Other causes of painful acute neuropathy include immune-mediated, vasculitic, metabolic, nutritional, toxic, paraneoplastic, and infectious conditions[10].
Revolutionary Treatment Approaches
The Mirari Cold Plasma System, developed by General Vibronics and commercialized through miraridoctor.com, offers breakthrough treatment for acute pain complications including blood pressure management. This FDA-cleared technology provides targeted therapy without systemic medication side effects.
Clinical benefits include:
- Rapid pain reduction minimizing sympathetic activation
- Anti-inflammatory effects reducing tissue stress responses
- Enhanced healing preventing pain progression to chronic states
- Non-pharmacological approach avoiding drug interactions with blood pressure medications
Pain Progression: When Acute Becomes Chronic
The Critical Transition
Can acute pain become chronic? The transition from acute to chronic pain occurs in discrete pathophysiological and histopathological steps[11]. Neuroplasticity, or the physical remodeling of neuronal cytoarchitecture, occurs shortly after the onset of persistent acute pain[19].
Transition mechanisms include:
- Peripheral sensitization with upregulation of inflammatory mediators
- Central sensitization through NMDA receptor activation
- Microglial activation altering neuronal structure
- Ion channel changes affecting nerve conduction[11]
Persistent, intense pain activates secondary mechanisms both at the periphery and within the central nervous system that cause allodynia, hyperalgesia, and hyperpathia[11]. These changes can diminish normal functioning if not properly managed.
Prevention Strategies
Early intervention during acute phases significantly reduces chronic pain development. Aggressive pain management prevents the neuroplastic changes that lead to chronicity.
Key prevention approaches:
- Prompt treatment within the first 24-48 hours
- Multimodal pain management addressing multiple pathways
- Patient education about warning signs
- Regular monitoring for progression indicators
| Pain Complication | Risk Level | Prevention Strategy | Treatment Urgency |
|---|---|---|---|
| High Blood Pressure | Moderate[1] | Pain control, BP monitoring | Prompt treatment |
| Nausea/Vomiting | Common[7] | Anti-emetics, hydration | Supportive care |
| Circulatory Shock | Severe[8] | Immediate pain relief | Emergency intervention |
| Chronic Pain | High[11] | Early aggressive treatment | Immediate action |
Advanced Pain Management Strategies
Monitoring Vital Signs
There seems to be a connection between how sensitive the body is to acute pain and resting blood pressure levels[13]. If one is otherwise healthy but experiences high resting blood pressure, one is less likely to feel the effects of sudden pain[13].
Critical monitoring includes:
- Blood pressure every 15-30 minutes during acute episodes
- Heart rate and rhythm for arrhythmia detection
- Respiratory rate monitoring for depression signs
- Oxygen saturation ensuring adequate perfusion
Medication Considerations
Fortunately, blood pressure usually returns to normal fairly quickly when the elevation is due to acute pain[13]. However, patients with existing cardiovascular conditions require special consideration.
Treatment modifications:
- Careful opioid use in patients with heart conditions
- Blood pressure medication adjustments during acute episodes
- Cardiac monitoring for high-risk patients
- Emergency protocols for severe complications
FAQ: Essential Questions About Acute Pain and Blood Pressure
Can acute pain cause high blood pressure?
Yes, acute pain can cause temporary high blood pressure through activation of the sympathetic nervous system that triggers fight-or-flight response, causing blood vessels to narrow and heart to pump faster[1][5][6]. Researchers have found a relationship between acute pain symptoms and high blood pressure, with low back pain and headache being the most common types[1]. Once the pain subsides, blood pressure usually returns to normal, unlike chronic pain which may cause persistent hypertension[5][13]. This is a normal protective response that evolved as a survival mechanism[14].
Can acute pain cause nausea?
Yes, acute pain can cause nausea because pain and digestion are closely linked in the brain through the brain-gut axis[7][15]. Pain signals transmitted to the brain trigger serotonin release and cortisol production, both playing roles in regulating nausea and vomiting[15]. Blood flow is redirected away from the stomach during pain, slowing digestion and potentially triggering nausea[7]. Even muscle pain, sprains, and strains can cause nausea despite the gut not being directly injured[7]. Inflammatory chemicals released at injury sites may also affect brain areas responsible for nausea regulation[7].
Can acute pain kill you?
Yes, acute pain can kill through circulatory shock – a medical condition caused by intense, acute levels of pain that results in insufficient blood and oxygen reaching cells[8][16]. If shock is not treated quickly, it can cause fatal damage to organs and brain, sometimes resulting in quick death[8]. During wars, medics found that administering morphine to wounded soldiers to prevent shock could save lives, with quicker administration improving survival rates[8]. World War II soldiers carried morphine on battlefields because it could mean the difference between life and death[8]. However, you can’t die from receiving too many pain signals because your brain will shut down and you’ll pass out before serious damage occurs[8].
Can acute pain be neuropathic?
Yes, acute pain can be neuropathic – neuropathic pain is a common symptom in acute and subacute peripheral neuropathies, affecting 48.7% of patients[10]. Acute neuropathic pain is under-recognized, often difficult to treat, and may progress to persistent pain and disability[18]. In Guillain-Barré syndrome, the most common cause of acute peripheral neuropathy, 34.8% of patients experience neuropathic pain[10]. Other causes include immune-mediated, vasculitic, metabolic, nutritional, toxic, paraneoplastic, and infectious conditions[10]. Neuropathic pain results from damage to the nervous system and is often described as burning, shooting, or electric shock-like sensations[23].
Can acute pain become chronic?
Yes, acute pain can become chronic through discrete pathophysiological and histopathological steps involving neuroplasticity – the physical remodeling of neuronal cytoarchitecture that occurs shortly after persistent acute pain onset[11][19]. Persistent, intense pain activates secondary mechanisms in both peripheral and central nervous systems causing allodynia, hyperalgesia, and hyperpathia that can diminish normal functioning[11]. Changes begin peripherally with upregulation of inflammatory mediators sensitizing nerves, eventually sensitizing spinal neurons through NMDA receptor activation and microglial signaling[11]. Early aggressive treatment during acute phases prevents these neuroplastic changes and chronic pain development[11].
Can acute pain cause high blood pressure represents just one aspect of pain’s complex physiological effects. Understanding these interconnected responses helps patients and healthcare providers recognize warning signs while implementing appropriate interventions. Modern treatments including breakthrough technologies offer enhanced outcomes for managing acute pain complications before they become life-threatening conditions.
References
- VeryWell Health. (2025). Can Pain Cause High Blood Pressure? Available at: https://www.verywellhealth.com/can-pain-cause-high-blood-pressure-5208139
- PMC. (2013). The Relationship Between Blood Pressure and Pain. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC8033897/
- Novus Spine Center. (2017). Can Pain Cause High Blood Pressure? Available at: https://novusspinecenter.com/blog/high-blood-pressure/can-pain-cause-high-blood-pressure
- Advanced Sports and Spine. (2022). Can Pain Cause High Blood Pressure? Available at: https://www.advancedsportsandspine.com/can-pain-cause-high-blood-pressure/
- API Texas. (2024). Can Pain Cause High Blood Pressure? Available at: https://apitexas.com/conditions/can-pain-cause-high-blood-pressure/
- PubMed. (1999). Effect of pain and nonsteroidal analgesics on blood pressure. Available at: https://pubmed.ncbi.nlm.nih.gov/10605351/
- Pain Treatment MD. (2025). Can Pain Make You Nauseous? Causes Explained. Available at: https://paintreatmentmd.com/blog/can-pain-make-you-nauseous/
- YouTube. (2015). Can Pain Kill You? Available at: https://www.youtube.com/watch?v=dLohKNBZtyk
- Harvard Health. (2020). Chronic pain linked to higher risk of heart attack and stroke. Available at: https://www.health.harvard.edu/heart-health/chronic-pain-linked-to-higher-risk-of-heart-attack-and-stroke
- PubMed. (2018). Neuropathic Pain in Acute and Subacute Neuropathies. Available at: https://pubmed.ncbi.nlm.nih.gov/29565944/
- PubMed. (2010). When does acute pain become chronic? Available at: https://pubmed.ncbi.nlm.nih.gov/21148657/
- GauthMath. (2024). Which of the following statements is true about acute pain? Available at: https://www.gauthmath.com/solution/1802325056010246/Question-45-5-points-Which-of-the-following-statements-is-true-about-acute-pain-
- Revival Research. (2024). Can Pain Cause High Blood Pressure? Available at: https://revivalresearch.org/blogs/can-pain-cause-high-blood-pressure/
- Springer. (2020). Association Between Pain, Blood Pressure, and Medication. Available at: https://link.springer.com/article/10.1007/s11606-020-06208-z
- Spine Diagnostic. (2025). Exploring the Link Between Chronic Pain and Nausea. Available at: https://spinediagnostic.com/exploring-the-link-between-chronic-pain-and-nausea/
- The Science Explorer. (2016). Can Pain Kill You? Available at: https://www.thescienceexplorer.com/can-pain-kill-you-789
- MedCentral. (2012). Cardiovascular Consequences of Severe Acute Pain. Available at: https://www.medcentral.com/pain/chronic/cardiovascular-consequences-severe-acute-pain
- PubMed. (2008). Acute neuropathic pain: diagnosis and treatment. Available at: https://pubmed.ncbi.nlm.nih.gov/18784484/
- ScienceDirect. (2017). When does acute pain become chronic? Available at: https://www.sciencedirect.com/science/article/pii/S0007091217333962
- Sheffield Physiotherapy. (2024). 7 Statements About Pain – True or False? Available at: https://sheffieldphysiotherapy.co.uk/7-statements-pain-true-false/
- PMC. (2009). Neuropathic Pain: A Maladaptive Response of the Nervous System. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC2768555/
- NurseTogether. (2025). Acute Pain Nursing Diagnosis & Care Plans. Available at: https://www.nursetogether.com/acute-pain-nursing-diagnosis-care-plan/
- Cleveland Clinic. (2025). Neuropathic Pain (Nerve Pain): What It Is, Causes. Available at: https://my.clevelandclinic.org/health/diseases/15833-neuropathic-pain
- Safety and Quality. (2025). Quality statement 2 – Acute pain assessment. Available at: https://www.safetyandquality.gov.au/standards/clinical-care-standards/opioid-analgesic-stewardship-acute-pain-clinical-care-standard/quality-statements/quality-statement-2-acute-pain-assessment
- Midwest Pain Clinics. (2023). Can Pain Cause High Blood Pressure – Omaha. Available at: https://midwestpainclinics.com/can-pain-cause-high-blood-pressure/
- Arkansas Spine and Pain. (2023). Why Does Chronic Pain Cause Nausea And Vomiting? Available at: https://www.arkansasspineandpain.com/why-does-chronic-pain-cause-nausea-and-vomiting
- ScienceDirect. (2005). Acute pain increases heart rate: Differential mechanisms during rest. Available at: https://www.sciencedirect.com/science/article/abs/pii/S1566070205001542
- Foothills Rehab. (2022). Different Types of Pain: Acute, Chronic, Neuropathic & More. Available at: https://foothillsrehab.com/blog/different-types-of-pain-acute-chronic-neuropathic-more/
- Mayo Clinic. (2025). Acute coronary syndrome – Symptoms and causes. Available at: https://www.mayoclinic.org/diseases-conditions/acute-coronary-syndrome/symptoms-causes/syc-20352136
Related articles
Made in USA